in section Oncology
The group of malignant tumors of the skin consists of three basic types of tumors: cancer, melanoma and sarcoma. About 90% of skin cancer tumors. The rest of the 10% fall on a variety of sources of development and histological structure of tumors, which include:
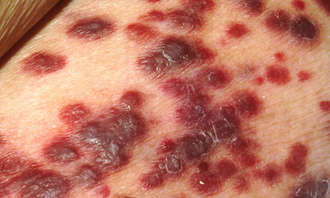 1), melanoma (malignant skin tumor pigmentnoobrazuyuschey system);
1), melanoma (malignant skin tumor pigmentnoobrazuyuschey system);
2) cancer of the skin appendages (adenocarcinoma of the sweat and sebaceous glands);
3) fibrosarcoma of the skin;
4) dermatofibrosarcoma protuberans skin;
5) skin leiomyosarcoma;
6) skin angiosarcoma;
7) multiple hemorrhagic Kaposi's sarcoma related, according to contemporary authors, for hematological malignancies.
The most common and represent the most practical significance of skin cancer and melanoma.
Skin cancer
Cancer of the skin with basal cell carcinoma is one of the most common forms of human malignancies and is the one in which the best results of treatment. Among the malignant tumors of skin cancer 12- 14% (3-5-place). The incidence of skin cancer ranges from up to 50 60, reaching a group of elderly people on 140-145 100 000 population. Deaths from skin cancer is relatively small and, as a rule, does not exceed 1-3 100 000 on residents. Skin cancer affects nearly the same proportion of men and women, the peak incidence of skin cancer refers to people aged up to 60 70 years.
Currently exogenous and endogenous factors nature, contribute to the occurrence of skin cancer, are combined into three large groups: 1) environmental factors; 2) chronic inflammation of the specific and non-specific nature of the phenomena of pathological regeneration; 3) pathological conditions of age or constitutional nature.
To environmental factors, primarily include long solar radiation. In addition, the exogenous causes of skin cancer are considered to be X-rays, exposure to other carcinogens, chronic physical trauma.
Skin cancer is often preceded by chronic inflammatory diseases, most often in nonhealing ulcers, scars and fistulas. The cancer may appear on the background of specific chronic inflammation associated with skin tuberculosis, syphilis, lupus erythematosus. Of skin cancer with chronic inflammation is usually preceded by a long period, sometimes for decades calculated.
A special group of factors for skin cancer include abnormal condition or age of a constitutional nature, which are called obligate precancer, that is almost always give rise to skin cancer. To obligate precancer are xeroderma pigmentosum, Bowen's disease and erythroplasia Keira.
On histological structure are two main forms of skin cancer: basal (basal cell skin cancer) and squamous cell carcinoma. Basal cell carcinoma is much more common - in 70-75% of cases, has a more favorable prognosis and almost always localized on the face (the inner corner of the eye, nosolobnaya region, temple, nostrils, nasolabial folds, the upper lip). Unlike skin cancer hits the mucous membranes. Basal cell carcinoma characterized by local destruirujushchego growth, almost metastasize.
Squamous cell carcinoma of the skin is divided into differentiated and undifferentiated and metastasizes lymphogenous by approximately 10% of patients with skin cancer. Hematogenous metastases occur rarely and only in the later stages of development of skin cancer. Especially malignant skin cancer occurs lower limbs, sometimes yielding in this respect, other sites of skin cancer.
Diagnosis of skin cancer is not too much difficulty, but sometimes it is necessary to carry out the differential diagnosis of chronic inflammatory diseases, such as tuberculosis, syphilis, deep fungal infection, and others. Crucial in the diagnosis of skin cancer belongs biopsy that skin cancer is almost safe. For small tumors, skin cancer produce a total excision of the pathological focus, and for large tumors of skin cancer take a piece of the tumor together with healthy surrounding tissue.
In the treatment of skin cancer using all the methods that are used for the treatment of malignant neoplasms: surgery, radiation, cryosurgery, local chemotherapy, laser therapy.
Treatment for Skin Cancer
Surgical treatment of skin cancer is most often used for tumors of the skin of the trunk and extremities, where there is a sufficient supply of skin. In squamous cell carcinoma, the incision should recede from the tumor edge by 1,5-2 cm, with basal cell not less than 0,5-1,0 cm from the visible boundaries of the lesion. The wider the tumor is removed, the lower the relapse rate. The surgical method is indicated for relapses, as well as for tumors that develop against the background of scars and fistulous passages. In a number of cases (bone germination, neurovascular bundle), localization of squamous cell carcinoma on the limb produces an amputation.
Radiation therapy is the primary treatment of skin cancer and the method of choice for its location on the scalp, and especially the face. The radiation sources may be blizkofokusnye radiotherapeutic installation and megavolt sources.
The most frequently used blizkofokusnaya radiotherapy using RUM-7, RUM-21, TOUR-60. Use an opportunity to change these devices penetrating ability of radiation when changing voltage generating X-rays (from the 10 100 to kV) depending on the extent of the process.
When basal cell carcinoma in the irradiation zone includes a tumor and surrounding at a distance 5 mm tissue to eliminate marginal recurrence. Irradiation is carried out with a single field, five times a week, single doses of 3-4 Gy total - 50-55 Gy.
For the treatment of squamous cell skin cancer irradiation field should be less than the visible boundaries of the tumor to see 1. Exposure mode is the same as in the treatment of Bazaleev, but the total dose brought to 60-65 Gy.
When common inoperable tumors applied remote gamma-therapy, electron radiation, or combined radiotherapy performed, including blizkofokusnuyu radiotherapy and remote gamma-therapy. The total dose at the same time make 60-65 Gy. Local radiation reaction when irradiated skin moist expressed epidermitis the end, or one to two weeks after exposure. Treatment epidermitis is applied topically and methyluracyl iruksolovoy ointments solcoseryl. Epithelialization usually occurs within 4-6 weeks.
Cryotherapy or destruction of tumor effect of low temperature used in skin lesions (usually basal cell carcinoma), located on the face, in cases where surgery can result in a cosmetic defect, and radiation therapy for some reason is not available. Cryosurgery is also used when you want to remove multiple tumors on the body.
Chemotherapy for cancer of the skin is used almost exclusively locally. Local chemotherapy is often used to treat recurrent basaliomas arising after surgery or radiation exposure, and the ointment is applied to the active anti-tumor agent (prospidin, omain et al.) On the tumor and the surrounding areas of healthy skin. Lubrication is made within 10-15 days that usually gives good therapeutic results.
Laser treatment of skin cancer in recent years become increasingly common. For laser irradiation, or laser treatment using different types of equipment (S02 lasers, helium-neon, helium-cadmium lasers and some others). Exposure is carried out under local or general anesthesia and is usually done in one session. A few days after the treatment forms a scab, which disappears in 3-4 weeks. Subsequently, scar formation that restricts the use of several laser for cosmetic problems.
Skin cancer has the best prognosis of all cancers. Basal cell carcinoma are cured in 95% of cases. When squamous cell carcinoma in the absence of regional metastases 5-year survival rate is 75-85%. The presence of metastases in regional lymph nodes and tumor ingrowth into the adjacent organs (T4, N1) reduce performance 5-year survival rate of up to 23-27%.
Melanoma
Melanoma skin - a relatively rare tumor (2-3% of the total number of human malignancies) that develops from pigment cells, melanocytes, which are located in the basal layer of the epidermis and produce the dark pigment melanin. The amount of melanin in your skin determines its color. In most patients, melanoma develops in place of some pigmented nevi, both congenital and acquired, although it can occur on externally unaltered skin.
Melanoma most often occurs in patients aged up to 30 60 years, men and women get sick at about the same frequency. Localization of melanoma varied, but often affects the lower limbs, trunk, rarely the head, neck and upper limbs. In most cases of melanoma are rare, multiple tumors are recorded in no more than 2-3% of patients.
Among the factors contributing to the emergence of melanoma is most commonly called solar radiation, since the frequency of these neoplasms is closely related to geography. However, unlike skin cancer, which most often occurs in places of greatest insolation, that is, in areas of former sunburn, melanoma does not always appear in these areas. In addition to external factors, genetic ones are also important. So, in blondes and especially red-haired melanoma occurs more often and prognostically proceeds more unfavorably. Increased frequency of melanoma in people with gray and blue eyes, as well as those who have different types of hyperpigmentation (freckles, birthmarks). It is noted that the consumption of animal products increases the risk of melanoma.
In the overwhelming majority of cases, malignant melanoma develops not on normal skin, but against the background of a congenital or acquired nevus. The most dangerous in terms of transformation into melanoma are the pigmentary border nevus, blue or blue nevus, the nevus Ota, the limited precancerous melanosis of Dubreia and some other, much rarer species. At the same time, many other non -oidal formations (pigmentary papillomatous, fibroepithelial, warty, intra-dermal nevi) generally do not give rise to melanoma or are malignant rarely.
There are symptoms of activation nevus, the totality of which can help the doctor suspect the beginning of malignancy or melanoma has arisen:
- rapid nevus growth, asymmetric increase or densification of one of its sections;
- change in nevus pigmentation;
- the appearance of new sensations in the area of the location of the nevus (tingling, itching, burning, tension);
- the appearance of papillomatous outgrowths, cracks, bleeding;
- hair loss from the surface of the nevus;
The emergence of new satellite nodules, increase in regional lymph nodes, melanuriya testify already developed melanoma, and are often manifestations of the generalization process.
In the diagnosis of malignant melanoma, in addition to the above clinical symptoms, radioisotope techniques help (the study with 32P, which accumulates in melanoma is 2-7 times more than in the symmetrical area of healthy skin) and thermography (melanoma temperature at 2-4 ° С above , Than in normal skin). However, the morphological study of the material obtained from melanoma is crucial. The main method is puncture biopsy or examination of smears-prints from the surface of an infected tumor. The danger of puncture melanoma thin needle is currently questioned, but this procedure still seek to maximize the next therapeutic effect. Usually puncture is performed after 2-3 irradiation sessions of melanoma. In cases where the cytological data of the puncture material are uncertain, total biopsy, i.e., excision of the tumor within healthy tissues, is performed, and an urgent histological examination is usually performed.
Histologically, there are four major cell types of melanoma: spindle cell, epithelioid, small cell and nevokletochny nevusopodabny. There are also mixed-polymorphocellular or melanoma.
Metastasis melanoma can be extremely varied, although as a rule, initially affected regional lymph nodes. Hematogenous metastases most often develop in the lungs, but may be affected and any other organs.
For the treatment of melanoma used a surgical, radiation, and combination drug methods, and laser therapy. The basic principle of modern surgery is radical removal of the primary tumor and regional metastases. The tumor is excised broadly within healthy tissue. The distance that a departure from the edge of the visible tumor, ranging from 2 cm (1 level of infestation by Clark) to 5-8 see when TK-T4. However, since the level of infestation becomes known only after the histological examination of the removed material, usually a surgical incision extends at least 5-6 cm from the edge of the tumor. At the initial stages of the disease the removal of regional lymph nodes unchanged prophylactic is now considered inappropriate. Radiation therapy as a component of combined treatment is more often used as a preoperative irradiation. Typically, this is used blizkofokusnaya radiotherapy, sometimes electron radiation. The dose fractions of 5-6 Gy brought to 50-60 Gy, and in terms of 1-2 days before 2-3 weeks after irradiation performed surgical stage. In cases where radiotherapy is used as an independent method, the dose to the primary tumor up 60-80 Gy to the regional lymph nodes - 45-50 Gy. Chemotherapy in its present form is unable to lead to permanent cure melanoma patients, but is widely used in various clinical situations. For disseminated disease forms, usually in combination with immunotherapy applied dimethyl-triaza-imidazol-karboksamin (DTIC), nitrosomethylurea (NMU). They are also used drugs such as prospidin, cyclophosphamide, vinblastine, vincristine, actinomycin D, bleomitsetin, penlomitsin and others. In 30-40% cases it is possible to achieve the objective regression of tumor lesions, even in generalized forms of melanoma. These drugs are used in the schemes of preventive chemotherapy for clinical stage III disease. In the treatment of melanomas of limbs the method of local chemotherapy in the form of extracorporeal perfusion anticancer drugs in high concentrations. Insulation made turnstile limbs and blood circulation is supported by heart-lung machine. Immunotherapy is widely used in a variety of treatment regimens of patients with melanoma. With active nonspecific immunotherapy are administered to a patient different vaccines (BCG, smallpox, pertussis, etc.)., Or immunomodulators (Poly A | U, levamisole et al.), Which increase the overall immunological activity. Sometimes the positive results achieved by the injection of vaccines to metastatic sites. Active specific immunotherapy aimed at enhancing immune responses when administered autologous and allogeneic tumor cells treated with various methods to reduce the likelihood of implantation metastases, but while retaining the antigenic structure. When passive immunotherapy in patients with generalized form of melanoma are administered serum immunized donors. Adoptive immunotherapy comprises administering to the patient immune cells (leukocytes, lymphocytes, bone marrow cells). The complexity of this type of treatment are antigenic differences between the cells of the patient and the donor. There are reports of positive results of treatment of melanoma by administering a patient's own lymphocytes treated with activators such as PHA, methotrexate, and others. Laser treatment of melanoma of the skin is used widely. Laser excision (SOG-lasers, neodymium laser) is used in the pigmented nevi, changes its state; Dyubreya melanosis, melanoma in situ and stage I; surface spread of melanoma. Excision is performed at a power output of 25-30 W focused to 0,3-0,5 mm beam, stepping back from the edges of the tumor on 3-5 see. After excision of the wound surface is irradiated with a defocused to 5-10 mm laser beam in order to achieve ablation and hemostasis. When the primary forms of melanoma (1 level of infestation by Clark) forecast of favorable, almost all of these patients can achieve stable recovery. With increasing depth of invasion of the tumor prognosis worsens and 5-th level of invasion five-year survival is less than 30- 40%. In the presence of metastases in regional lymph nodes, regardless of the size of the primary tumor, the survival rate is not more than 15-25%.
В Kiev Center for Fungotherapy, Bioregulation and Ayurveda qualified doctors of alternative medicine are receiving. Cost of consultation 300 UAH. You can look at medical histories and treatment results on this link.
You can make an appointment by phone: (097) 231-74-44, (050) 331-74-44, (063) 187-78-78, +38 (098) 583-85-85 (Viber), +38 (093) 688-25- 88 (WhatsApp, Telegram) Email:This email address is being protected from spambots. You need JavaScript enabled to view it.

















 Many messenger users use the Telegram application, as, unlike Viber, new members of the group can see the previous correspondence in the group. To join the "Alternative Medicine" group in Telegram, scan the QR code or follow the invitation link
Many messenger users use the Telegram application, as, unlike Viber, new members of the group can see the previous correspondence in the group. To join the "Alternative Medicine" group in Telegram, scan the QR code or follow the invitation link 







